
Meniscus injuries disrupt knee biomechanics, often compensated within a year, as detailed in recent protocols and research from 2018-2025.
Effective rehabilitation, including post-surgical care, focuses on pain management and restoring function, utilizing protocols like those found in available PDF resources.
Contralateral electromyostimulation aids recovery, reducing pain and improving mobility, while comprehensive programs address ligament injuries alongside meniscus repair.
Understanding the Meniscus and its Function
The menisci, two C-shaped fibrocartilage structures within the knee joint, are crucial for shock absorption, load distribution, and joint stability. They enhance congruity between the femur and tibia, minimizing stress on the articular cartilage and preventing early osteoarthritis. Understanding their biomechanical role is paramount when designing rehabilitation protocols, often detailed in meniscus injury exercises PDF guides.
These structures aren’t simply passive cushions; they actively contribute to knee function during movement. Damage, whether acute or degenerative, disrupts this delicate balance. Research from 2022, citing 42 studies, highlights the impact of pain perception on procedural outcomes, emphasizing the need for early pain management strategies integrated into rehabilitation. Effective protocols, like those referenced in available PDF resources, aim to restore optimal biomechanics, compensating for the initial disruption, as observed in cases resolving within a year.
Proper function allows for smooth, pain-free movement, while injury leads to pain, swelling, and limited range of motion; Therefore, targeted exercises, often outlined in meniscus repair rehabilitation protocols, are essential for restoring the meniscus’s vital role.
Common Causes of Meniscus Injuries
Meniscus tears frequently occur due to twisting or pivoting motions, particularly during sports activities. Direct impacts, like those experienced in contact sports, can also cause damage. Degenerative changes, associated with aging, increase susceptibility to tears even with minimal trauma. Understanding these mechanisms informs the development of preventative and rehabilitative strategies, often detailed in meniscus injury exercises PDF resources.
Surgical procedures themselves can sometimes contribute to injury, highlighting the importance of meticulous technique and post-operative rehabilitation. Pain perception during and after procedures, as noted in research from 2022, influences recovery, emphasizing the need for comprehensive pain management. Protocols, available as PDF guides, address both acute and chronic injury scenarios.
Rehabilitation programs, like those analyzed in studies from 2025, aim to restore function and prevent re-injury. These programs, often found as meniscus repair rehabilitation protocols, focus on strengthening supporting muscles and improving proprioception.

Phase 1: Immediate Post-Injury (0-2 Weeks)
Initial focus is pain and swelling control, utilizing RICE (rest, ice, compression, elevation) as outlined in meniscus injury exercises PDF guides.
Goals of Phase 1 Rehabilitation
The primary objectives during the initial 0-2 week phase, detailed in meniscus injury exercises PDF protocols, center around minimizing pain, reducing swelling, and protecting the injured knee joint. A crucial goal is restoring a basic range of motion without exacerbating the injury, achieved through gentle, pain-free movements.
Early intervention aims to prevent muscle atrophy, particularly in the quadriceps, which rapidly weakens after injury. Maintaining some level of muscle activation is vital for long-term recovery. Furthermore, Phase 1 focuses on establishing proper neuromuscular control, preparing the knee for subsequent strengthening exercises.
Importantly, this phase prioritizes patient education regarding activity modification and weight-bearing restrictions, as outlined in rehabilitation guides. The ultimate aim is to create a stable foundation for progressing through the rehabilitation program, avoiding re-injury and optimizing functional outcomes, referencing research from 2021-2025.
Exercises for Phase 1: Range of Motion & Pain Control
Initial exercises, as detailed in meniscus injury exercises PDF resources, emphasize gentle range of motion (ROM) exercises. These include heel slides, performed lying down, and assisted knee flexion, gradually increasing the bend. Ankle pumps are crucial for reducing swelling and promoting circulation. Quadriceps sets – tightening the thigh muscles – help maintain muscle activation without stressing the joint.
Pain control strategies involve RICE (Rest, Ice, Compression, Elevation). Ice application, 15-20 minutes several times daily, minimizes inflammation. Gentle patellar mobilizations can prevent stiffness. Weight-bearing is initially limited, often requiring crutches, guided by pain levels.
These exercises, often outlined in post-surgical protocols from 2022 and 2025, are performed slowly and deliberately, stopping at the onset of pain. The focus is on regaining basic movement and reducing discomfort, preparing the knee for more advanced rehabilitation phases.

Phase 2: Early Strengthening (2-6 Weeks)
PDF protocols emphasize quadriceps and hamstring strengthening, progressing from isometric holds to short-arc exercises, building foundational knee stability.
Progressing Exercises: Focus on Quadriceps & Hamstrings
PDF rehabilitation guides detail a structured progression for quadriceps and hamstring strengthening, crucial during weeks 2-6 post-injury or surgery. Initial exercises, often outlined in downloadable protocols, involve straight leg raises – both sets and repetitions are carefully prescribed to avoid overstressing the healing meniscus;
As pain subsides, short-arc quads and hamstring curls are introduced, utilizing resistance bands or light weights. These exercises target specific muscle groups without placing excessive strain on the knee joint. Emphasis is placed on controlled movements and proper form, as detailed in available resources.
Progressive overload is key; gradually increasing resistance and repetitions as tolerated. Wall squats and step-ups (low height) are incorporated cautiously, monitoring for any signs of discomfort or swelling. The goal is to rebuild muscle strength and endurance, preparing the knee for more advanced exercises in subsequent phases, as described in comprehensive meniscus injury exercises PDF documents.
Proprioceptive Exercises for Knee Stability
Proprioception, the body’s awareness of its position in space, is vital for knee stability post-meniscus injury. PDF rehabilitation protocols emphasize exercises to restore this sense, often beginning with simple weight shifts while standing on a stable surface. These are foundational, preparing the knee for more challenging activities.
Single-leg stance, initially with eyes open and then closed, is a common progression, enhancing balance and neuromuscular control. Wobble boards and balance discs are frequently incorporated, as detailed in downloadable guides, to challenge stability further.
These exercises improve the knee’s ability to react to unexpected movements, reducing the risk of re-injury. The focus is on controlled, slow movements, engaging the surrounding muscles to stabilize the joint. Consistent practice, guided by a physical therapist and outlined in meniscus injury exercises PDF resources, is crucial for regaining full functional capacity.

Phase 3: Intermediate Strengthening (6-12 Weeks)
PDF protocols detail advanced exercises like lunges and step-ups, building strength and endurance. Agility drills introduce lateral movement, progressing rehabilitation effectively.
Advanced Strengthening Exercises: Lunges & Step-Ups
Lunges and step-ups are crucial components of intermediate meniscus rehabilitation, detailed within comprehensive PDF protocols. These exercises progressively load the knee joint, enhancing quadriceps, hamstrings, and gluteal strength – vital for dynamic stability.
Begin with controlled movements, focusing on proper form to avoid re-injury. Initially, perform these exercises without added weight, gradually increasing resistance using dumbbells or resistance bands as strength improves. PDF guides often recommend starting with a limited range of motion, progressively increasing it as pain allows.
Variations, such as forward, reverse, and lateral lunges, challenge the knee in different planes of motion. Step-ups onto a low platform build single-leg strength and endurance. Remember to prioritize controlled descent and ascent, maintaining proper alignment throughout each repetition. Consistent adherence to a structured program, as outlined in rehabilitation PDFs, is key to successful recovery.
Introducing lateral movement is a pivotal step in advanced meniscus rehabilitation, often detailed in specialized PDF protocols. Agility drills rebuild neuromuscular control and prepare the knee for the demands of daily activities and sports. Begin with simple exercises like side shuffles and carioca, emphasizing controlled movements and maintaining a stable knee position.
Cone drills and figure-eight runs progressively challenge agility and coordination. These drills should be performed with a focus on quick footwork and minimal valgus or varus stress on the knee. PDF resources frequently suggest starting with a wider base of support and gradually narrowing it as confidence and strength increase.
Proper warm-up and cool-down are essential to prevent re-injury. Remember to listen to your body and modify exercises as needed, adhering to the guidelines provided in your rehabilitation PDF.

Phase 4: Return to Activity (12+ Weeks)
Sport-specific training, guided by PDF protocols, gradually reintroduces demands; functional exercises assess readiness, ensuring safe return to play after meniscus repair.
Sport-Specific Training & Functional Exercises
Transitioning back to activity requires a carefully structured program mirroring the demands of the individual’s sport, often detailed within comprehensive meniscus injury exercises PDF guides.
This phase emphasizes replicating movements encountered during gameplay, progressively increasing intensity and complexity. For example, a runner will focus on interval training, agility drills, and distance running, while a basketball player will incorporate jumping, pivoting, and shooting drills.
Functional exercises assess the knee’s ability to handle real-world scenarios. These include hop tests (single-leg and lateral), shuttle runs, and cutting maneuvers. PDF resources often provide standardized testing protocols to objectively measure progress.
The goal isn’t simply to regain strength, but to restore neuromuscular control and proprioception – the body’s awareness of its position in space. This minimizes the risk of re-injury. Rehabilitation protocols, as highlighted in recent research (2021-2025), stress the importance of a gradual, progressive approach, guided by pain levels and functional testing results.
Criteria for Return to Play
Returning to sport post-meniscus injury isn’t solely based on time elapsed; objective criteria, often outlined in detailed meniscus injury exercises PDF protocols, are paramount. These protocols, informed by research from 2018-2025, emphasize a phased approach.
Key criteria include full, pain-free range of motion, symmetrical quadriceps and hamstring strength (typically >90% compared to the uninjured leg), and successful completion of functional hop tests. Neuromuscular control and proprioception must also be restored.
Specific tests may include a single-leg hop for distance, a triple hop for distance, and a timed agility shuttle run. PDF guides often provide normative data for comparison. Absence of swelling or effusion post-exercise is crucial.
Ultimately, a physician and physical therapist must jointly determine readiness, considering the athlete’s individual circumstances and the demands of their sport. Rushing the return increases re-injury risk, potentially negating prior rehabilitation efforts. A conservative, evidence-based approach is essential.

Important Considerations & Precautions
Pain management is vital; PDF protocols detail strategies, while careful monitoring prevents re-injury, ensuring adherence to rehabilitation phases for optimal healing.
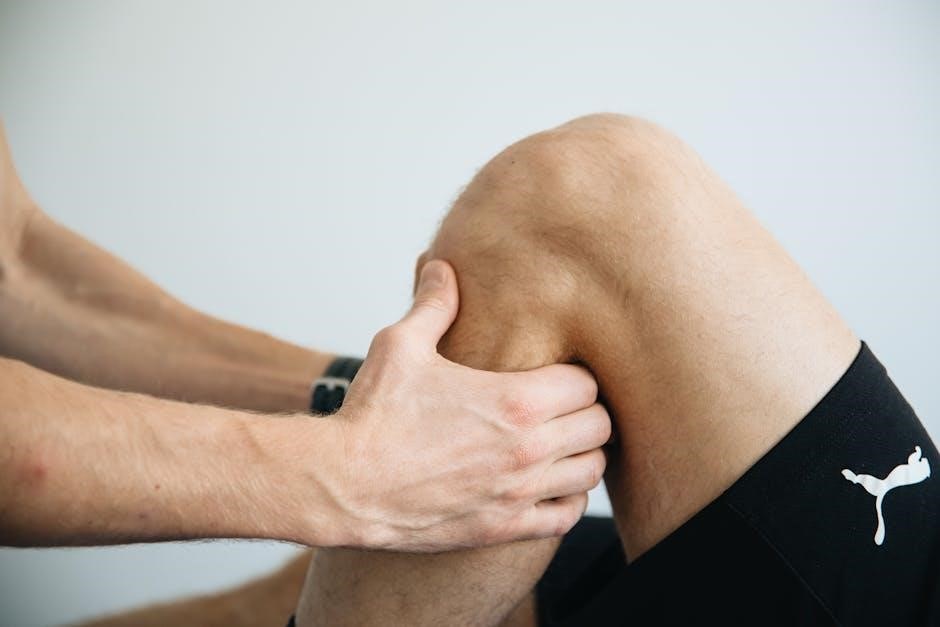
Pain Management Strategies
Effective pain control is paramount throughout meniscus injury rehabilitation, as highlighted in numerous PDF protocols and recent research (2022, 2025). Initial strategies often involve RICE – Rest, Ice, Compression, and Elevation – to minimize acute inflammation and discomfort. Pharmacological interventions, such as over-the-counter pain relievers or, in some cases, prescription medications, may be recommended by a physician.
However, a holistic approach is crucial. Rehabilitation protocols emphasize gradual loading and controlled movements to desensitize the knee joint and reduce pain perception. The perception of pain is affected by pre-procedure intensity, influencing treatment effectiveness. Furthermore, incorporating contralateral lower-limb electromyostimulation, as suggested by studies, can facilitate earlier recovery and pain reduction.
Consistent adherence to prescribed exercises, even when discomfort is present (within tolerable limits), is essential for long-term pain management and functional restoration. Regular monitoring and communication with a physical therapist are vital to adjust the program based on individual pain levels and progress.
Preventing Re-Injury
Re-injury prevention is a critical component of long-term meniscus injury recovery, detailed within comprehensive rehabilitation PDF guides and research from 2018-2025. A successful return to activity necessitates addressing biomechanical imbalances and restoring optimal knee stability. Protocols emphasize progressive strengthening of the quadriceps, hamstrings, and calf muscles, crucial for dynamic knee control.
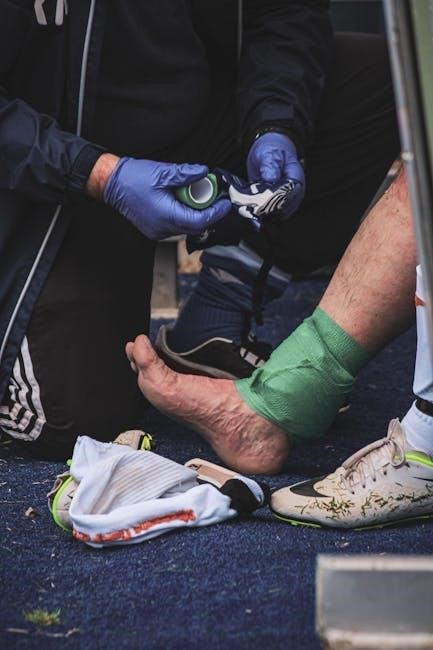
Proprioceptive training, focusing on balance and joint position sense, is vital to enhance neuromuscular control and reduce the risk of re-trauma. Adhering to a structured return-to-sport program, gradually increasing activity levels, is paramount.
Furthermore, maintaining consistent exercise habits, even after completing formal rehabilitation, helps preserve strength and stability. Understanding proper biomechanics during functional movements, and addressing any persistent gait abnormalities, are essential. Ignoring pain signals and prematurely returning to high-impact activities significantly increases the likelihood of re-injury.
Resources & Further Information
PDF protocols from 2018-2025 offer detailed meniscus repair guidance; consult a qualified physical therapist for personalized exercise plans and optimal recovery strategies.
Finding a Qualified Physical Therapist
Locating an experienced physical therapist is crucial for successful meniscus injury rehabilitation. Seek professionals specializing in orthopedic conditions, specifically knee injuries, and possessing advanced certifications in manual therapy or sports rehabilitation.
Verify their credentials and experience through professional organizations and online reviews. A skilled therapist will conduct a thorough evaluation, tailoring an exercise program based on your injury’s severity, surgical history (if applicable), and individual needs.
Effective therapists utilize evidence-based practices, incorporating progressive exercises detailed in PDF rehabilitation protocols from sources like those published between 2018 and 2025. They’ll monitor your progress, adjusting the program to ensure optimal recovery and prevent re-injury.
Don’t hesitate to ask about their experience with meniscus repair protocols and their approach to pain management. A strong therapist-patient relationship built on clear communication is essential for achieving your rehabilitation goals.
Recommended PDF Resources for Meniscus Repair Protocols
Numerous PDF resources detail meniscus repair rehabilitation protocols, offering valuable guidance for patients and therapists. While specific documents weren’t directly linked, research from 2018 to 2025 indicates the availability of comprehensive guides.
Search for protocols from reputable orthopedic institutions and sports medicine clinics. Look for documents outlining phased rehabilitation programs, including range-of-motion exercises, strengthening routines, and proprioceptive drills.
Resources often detail post-operative timelines, specifying exercise progressions and criteria for advancing to each phase. Pay attention to protocols addressing pain management strategies and precautions to avoid re-injury.
Consider searching for guides related to ACL reconstruction recovery, as these often include detailed meniscus rehabilitation components. Remember to discuss any PDF-sourced exercises with your physical therapist to ensure they align with your individual needs and recovery progress.